Do you have pain in your pelvis, buttocks or into your legs around the time of your period? Has pelvic pain and fullness affected your ability to enjoy intimacy or live life to its fullest? If so, you may have pelvic vein disease or pelvic congestion syndrome.
Pelvic vein disease and its symptoms are often misunderstood. They can affect your quality of life and prevent you from living a fulfilling life. It is not right if you are suffering in silence and feel like your symptoms are being ignored by your doctors. We are here to help you.

Pelvic pain can be a vexing problem. Almost one third of women with chronic pelvic pain have pelvic vein disease, the majority of whom are 45 years old or younger. Other risk factors for pelvic vein disease include polycystic ovarian syndrome (PCOS), multiple pregnancies, hormonal dysfunction, fullness of leg veins, or weight gain.
Typical pelvic vein symptoms are related to varicosities in veins in the area of your uterus and ovaries. Defective vein check valves allow blood to pool in the pelvic veins, resulting in dull pain, heaviness, and pressure. As the pelvic veins become varicose, reflux can extend into branches that connect with varicose veins in the inner thigh, labial and buttock areas.
Primary sources of pelvic vein disease are the left renal, ovarian, and common iliac vein. Other veins in the lower abdomen and pelvis may contribute to your symptoms. Pelvic vein disease may also develop in patients with a history of deep vein thrombosis (DVT) and scarring of the iliac veins.
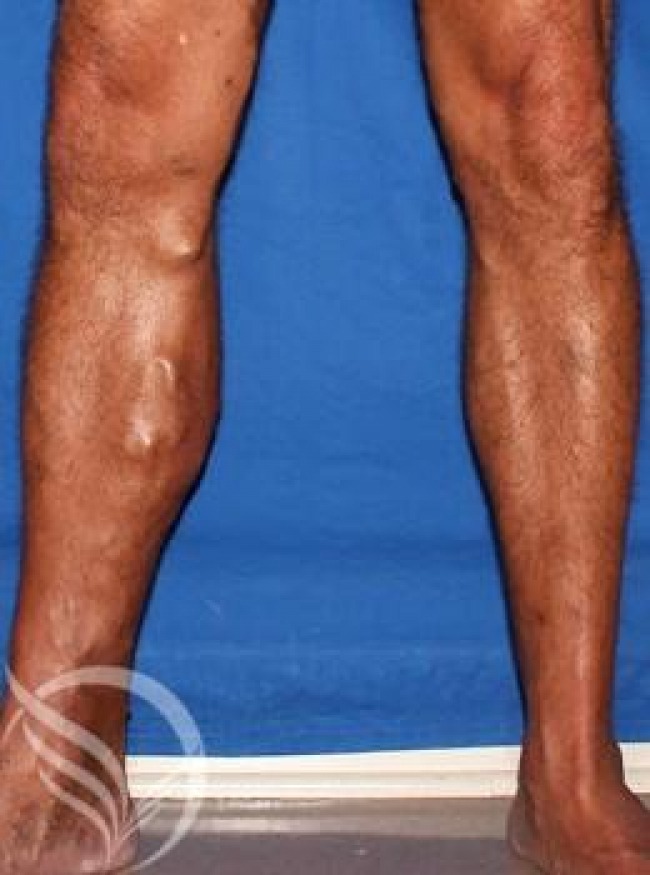
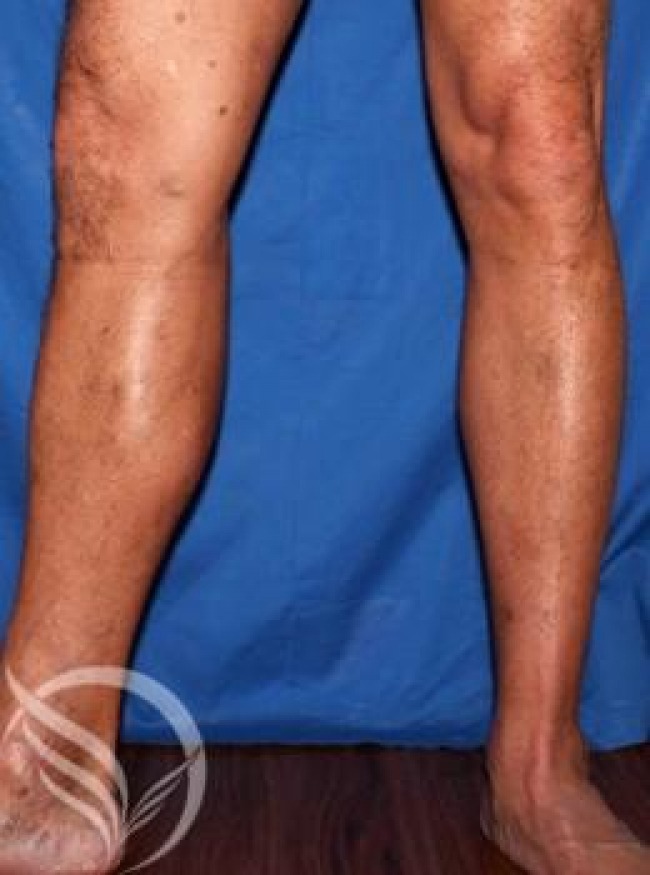
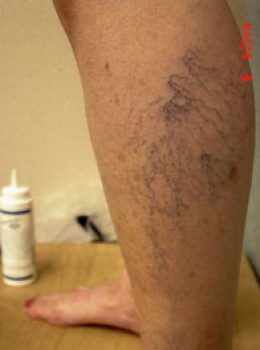
Your treatment recommendations are based on your symptoms, physical findings and the results of your vein mapping diagnostic ultrasound.
If your pelvic symptoms are limited, you are considering having another child, or your primary symptoms are leg varicose veins, you may choose to treat your leg veins first. If you have an early recurrence of varicose veins (12-18 months) after your vein procedure, an evaluation for pelvic vein disease would then be recommended before additional treatment of the recurrent varicose veins.
If your pelvic vein disease is significant, and affecting your quality of life, you may choose to evaluate and treat the pelvic vein disease first. In that situation, a transabdominal ultrasound of the abdomen and pelvic veins is ordered. Based on that study, the next step would be a pelvic and iliac vein evaluation, often with the intent to treat.
The pelvic and iliac vein evaluation includes a venogram and intravascular ultrasound (IVUS), often with intent to treat. The studies evaluate the common sources of pelvic vein disease left and right iliac veins, left renal vein, and both ovarian veins.
Based on the patterns of reflux seen at the time of your evaluation, a treatment plan is recommended to correct your issues. In most circumstances this can be done at the same time as the venogram and IVUS. Those details will be discussed with you prior to your evaluation.
The left ovarian vein study includes an evaluation of the left renal vein. If the renal vein is contributing to the ovarian vein reflux, other considerations that would be discussed with you prior to proceeding with treatment. If there is isolated reflux in your ovarian vein, the treatment is to close the refluxing vein segment. The unhealthy refluxing ovarian vein treatment is performed under venogram guidance with the injection of sclerosing foam, and coils to collapse the diseased vein segment. Blood flow is redirected to healthier veins located nearby.
If your primary problem is disease in the left common iliac vein, intervention may include dilation of the scarred segment of the iliac vein with or without stents to hold the vein open. When there is combined iliac and ovarian vein reflux, the sequencing of treatment will be discussed with you.


It’s just 3 easy steps…



Treatments are Walk in. Walk out® performed in our outpatient imaging center. We keep you comfortable and monitor your vitals during the study. You may feel a slight pinch from the local anesthesia at the IV site, followed by pressure from the IV catheter insertion. When the venogram contrast solution is injected, you may feel a warm flush. The evaluation and treatment processes are guided by ultrasound and fluoroscopic x-ray. A band-aid is placed at the IV site when we are done. The results of the study, your treatment, and ongoing plans will be discussed with you.
Discomfort following the treatment is controlled with oral OTC or prescription medication. Over the coming days and weeks, symptoms should gradually improve, as the venous blood flow normalizes. Periodic abdominal/pelvic ultrasounds will be needed to follow the treated vein. Since vein disease is a chronic condition, additional treatment may be needed in the future.
It is recommended patients receiving ovarian vein embolization and/or iliac vein stenting, rest and recover for 1 week after the procedure. After that, as you feel better, you may begin to resume normal activities. Both minimally invasive techniques are a fantastic alternative to more invasive treatments used in the past.
Vein Specialists of the South have cultivated the reputation as a leader in vascular health. We are proud to have served more than 30,000 patients. If you are concerned about a vascular issue, there’s no one better to restore your veins to full health than Vein Specialists of the South.
Receive a FREE resource via email about non-surgical treatments and how we can help.

Since 1997, Vein Specialists of the South has helped thousands of patients like you with varicose veins, spider veins, and leg swelling. Dr. Kenneth Harper is a leader in vein health is a Diplomat of the American Board of Surgery and the American Vein and Lymphatic Medicine. Terri Harper, MSN, FNP-C, is a renowned educator in the field of cosmetic sclerotherapy. Our dedicated nurse injectors have been trained by the best.
At Vein Specialists of the South, we have a passion for veins – big and small. We’ve helped over 30,000 people get Better Veins for Life®. Call today to schedule an appointment with the VSS team, where ‘Veins Aren’t Just One Thing We Do, They Are the Only Thing We Do.®’
Meet with your dedicated vein care specialists to get started on your personalized comprehensive treatment plan.

*Individual Results May Vary

556 3rd Street, Suite A
Macon, Georgia 31201
4851 Bill Gardner Pkwy,
Locust Grove, GA 30248
151 South Houston Lake Rd
Warner Robins, Georgia 31088
© Copyright 2024 Vein specialists of the south | Terms of Use | Website Privacy Policy | Medical Privacy Policy
Complete the information below to receive a Receive a FREE resource about non-surgical treatments and how we can help.
Ready to learn how we can help you enjoy Better Veins for Life®?
Complete the information below to receive a FREE resource about varicose veins.