The Potential Consequences Of Ignoring Venous Disease
Are varicose veins dangerous? The short answer: sometimes.
Not all varicose veins require treatment, but if you have them you should see a vein specialist. Some varicose veins can be managed with lifestyle changes that prevent them from advancing. These “Better Veins for Life Principles” include: wearing medical grade graduated compression socks, taking a break for leg elevation several times per day, maintaining your healthy weight, and a regular exercise routine.
However, some varicose veins are more severe and require medical treatment. By the time most people see a vein specialist for their varicose veins, their veins are already large, bulging, and painful. At this point, the odds of developing a secondary condition have increased.
This article aims to educate you about the sometimes dangerous consequences of not having your varicose veins evaluated, monitored, and treated by a trained vein specialist.

Are Varicose Veins Dangerous If Not Evaluated, Monitored, And Treated?
While not all varicose veins are dangerous, they should be evaluated and monitored by a vein specialist to determine the scope of treatment required every step of the way. This helps prevent secondary issues related to varicose veins, which include spontaneous bleeding, blood clots, inflammation, venous ulcers, and more.
Bleeding Varicose Veins
Bleeding varicose veins can occur after minimal trauma with tearing or bursting of a vein. The injury does not have to be severe, but can be as simple as brushing up against the edge or corner of a piece of furniture, or even scrubbing a little too hard in the shower.
If the skin is not broken, the injury causes a bruise. However, if the skin is broken at a varicose vein there can be a great deal of blood loss, causing patients to rush to the emergency room to stop the bleeding. The bleeding can be emotionally traumatizing, dangerous, and the emergency room visit is expensive. Seeking treatment for your varicose veins before the injury and bleeding occurs makes good sense.
Varicose Veins And SVT And DVT Risk
Venous blood must flow to prevent clotting. Once blood flow slows, the risk of clotting increases. Clotting is a normal response to limit the loss of blood during an injury. However, the pooling of venous blood with varicose veins can cause the veins to clot creating an SVT, or Superficial Vein Thrombosis.
Decreased blood flow through a varicose vein, blood clotting, and vein damage all contribute to a venous inflammation called superficial thrombophlebitis. This inflammation is just below the surface of the skin, causing red, tender masses, with leg pain over the varicose veins.
If a clot forms in the deep vein of the leg it is called a DVT, or Deep Vein Thrombosis. Blood clots in the legs are often asymptomatic but they can cause pain, swelling, and difficulty walking. Additionally, blood clots can break free and travel through the bloodstream to the lungs, causing a life threatening Pulmonary Embolism (PE). While PE can be treated with emergency medical attention, it can be fatal. PE is responsible for 1 death every 5 minutes in the US, many of which could be prevented.
Varicose Veins And Leg Ulcers
When varicose veins are left untreated, the pressure and inflammation from fluid buildup in the area can lead to skin changes and an open sore that can become infected. About 80% of skin ulcers in the lower leg are caused by varicose veins. Leg ulcers most often occur just above the ankle and are difficult to treat and heal. Without treatment, the infection can spread.
Lipodermatosclerosis And Venous Disease
Lipodermatosclerosis, not to be confused with lymphedema, is an inflammation of subcutaneous fat (the fat just beneath the skin) with skin hardening, uneven skin pigmentation, redness,and swelling; the condition is also painful for many patients. Although doctors are unclear on the exact cause, lipodermatosclerosis is more often found in patients who are obese and/or have varicose veins.
 When To See A Doctor About Varicose Veins
When To See A Doctor About Varicose Veins
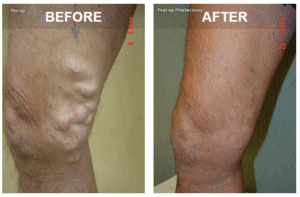
If you suspect this venous disease, you should speak to a vein specialist for a venous evaluation. Not all varicose veins are visible as the dark or bulging veins you see in before and after photos. Some are visible and less noticeable, while others aren’t seen at all. If you have unexplained leg pain or heaviness in the legs, you should be evaluated. An ultrasound can locate venous insufficiency, allowing our providers to address the problem effectively.
Patients in higher risk categories should also be routinely evaluated, especially if they notice symptoms of venous disease such as heaviness, aching, swelling, tenderness, burning and itching. Patients who are at an increased risk have a family history of venous disease, are of advanced age, and women over 30 who have had three or more children or who are taking oral contraceptives.
It isn’t just women and the elderly, however. If you sit or stand still for long periods of time, your risk for developing venous disease increases. If you’re on extended bed rest for any reason, you’re chances of developing blood clots go up as well.
Reduce The Risk Of Venous Disease At Vein Specialists Of The South In Middle Georgia
At Vein Specialists of the South in Middle Georgia and Central Georgia, we evaluate, diagnose, manage, and treat venous disease all day, every day. We specialize in spider veins, varicose veins, blood clots, and leg ulcers.
Are varicose veins dangerous? Getting them taken care of by a team of qualified, well-trained vein specialists decreases the likelihood of dangerous secondary conditions. Contact our team today for a consultation and reduce your risk of dangerous health consequences.