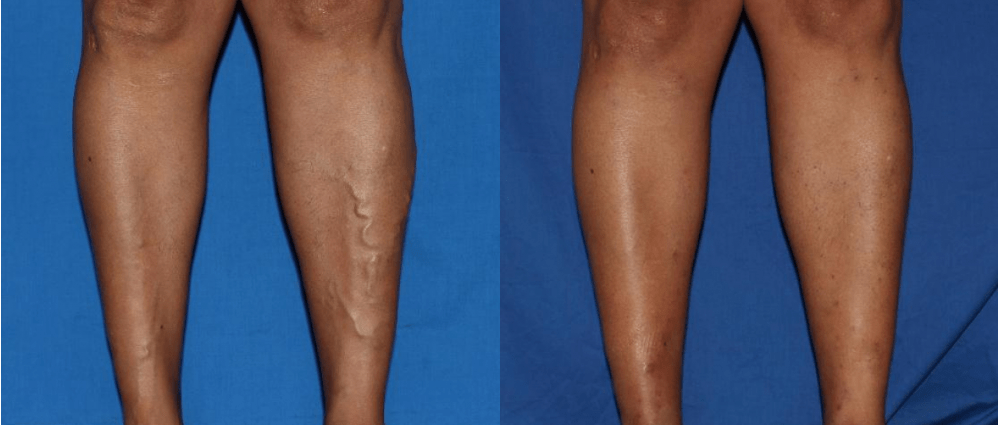
Why Do Varicose Veins Appear During Pregnancy?
Most people think varicose veins in pregnancy are triggered by weight gain, as your baby grows. However, the changes of pregnancy which increase your risks begin shortly after conception and continue, as your baby develops. Early in pregnancy, your blood volume increases to deliver nutrients and oxygen to support you and your developing baby. Hormonal changes follow that relax the ligaments and smooth muscle in preparation for delivery. These changes and others can cause your veins to dilate, putting a strain on your vein flow.
As you near delivery and afterward for about 12 weeks, your body’s natural blood clotting properties increase to limit bleeding during and or after delivery. When you consider these factors it is easy to see why the risks of varicose veins and blood clots increase during pregnancy and persists for at least 12 weeks after delivery.
The good news is there is hope. With lifestyle changes, your risks can be lowered. Over the first three months after your baby is born, some of the vein damage may reverse. And for those veins that persist there are effective, minimally invasive treatment options for you.
The more you know about healthy vein care the better prepared you will be during this special time in your life. Follow your Vein Specialists of the South healthy vein tips today and lower your varicose vein risks from the first trimester all the way through delivery and beyond.
How to Prevent Varicose Veins in Pregnancy
To lower your risks of developing varicose veins during pregnancy, there are guiding principles to help you. The first is regular exercises such as walking, swimming, and yoga. It is also important to stay well hydrated in order to keep your veins properly supplied with oxygenated blood. A healthy diet is important for your baby’s development and to avoid unnecessary weight gain for you. Another pointer is to elevate your legs several times a day to avoid swelling.
What you wear matters, too. Comfortable clothing that doesn’t pinch or constrict will allow for healthy circulation. We highly recommend you begin to wear compression socks and stockings as soon as you know you’re expecting. Compression socks and stockings are an essential part of preventing varicose veins during pregnancy.
Medical grade graduated compression helps overcome the negative influences of pregnancy on your vein flow improving circulation by augmenting the venous flow back toward the heart. A byproduct of this is reduced blood pooling in your legs, less swelling, and lowered risks of blood clots, which is one of the main causes of varicose veins.
By following these tips and taking proper care of yourself throughout your pregnancy, you can help prevent varicose veins and enjoy a healthier pregnancy.
However, if you notice any symptoms of varicose veins, discuss them with your OBGYN and reach out to our vein specialists for an evaluation.
Your VSS Better Veins for Life principles are as follows:
- Compression is key. If you didn’t wear compression, doing so now will help alleviate the symptoms while potentially preventing the worsening of your vein symptoms.
- Elevate your legs. Every OBGYN will tell you that you should elevate your legs during pregnancy. This is true if you have varicose veins as well. Allow gravity to assist healthy circulation from your feet back up to your heart.
- Exercise. Walking, swimming, and other low-impact activities can help alleviate the discomfort of varicose veins while also actively improving your circulation. Even pumping your calf muscles while sitting down will improve circulation and reduce venous symptoms.
- Don’t wear high heels. We realize most pregnant women opt for more comfortable shoes, but if you’re still wearing high heels, we highly recommend you set them aside for now. If you need something fashionable, there are lovely flats that will give you the look you want without affecting your vein health.
- Our fifth and final tip is to maintain a healthy weight, but this does not so much apply during pregnancy. If you have concerns about your pregnancy weight gain, discuss this with your OBGYN.